Covid vaccine: UK decision to delay second dose vindicated by new research
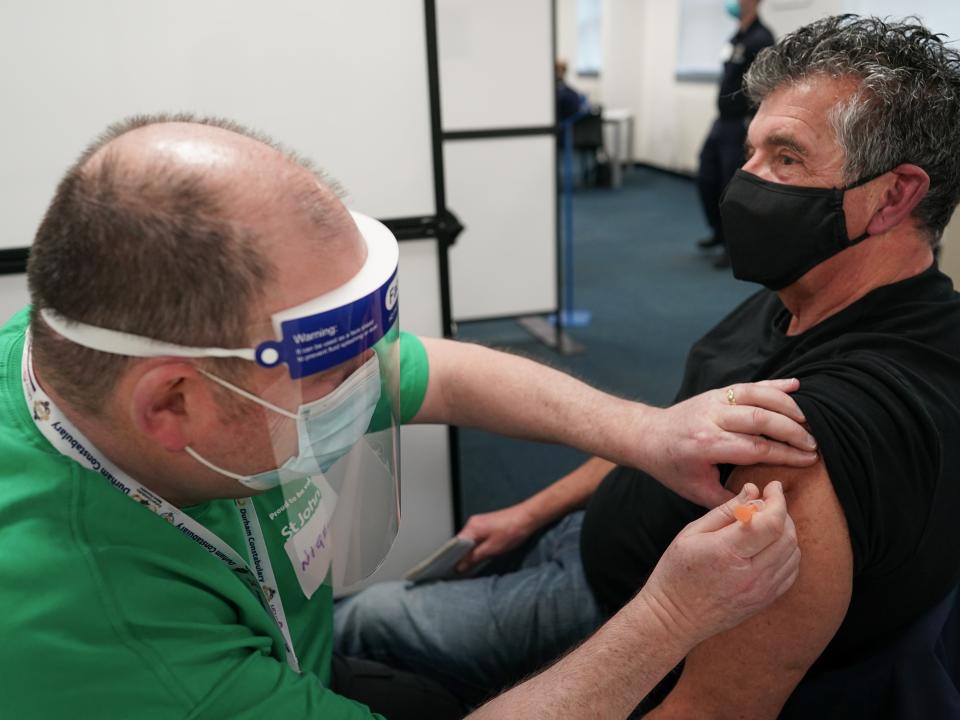
The UK’s decision to delay the administration of second Covid vaccinations has been vindicated by new research which suggests that the policy saves more lives than the standard dosing schedule.
Delaying the second dose so that more people can receive a first shot could reduce deaths by up to a fifth, according to new modelling from US experts.
Published in the British Medical Journal (BMJ), one example showed that if a first dose offered 80 per cent protection against Covid, deaths fell to 207 per 100,000 people if the second dose was delayed.
This compared with 233 deaths if people received their second dose after three to four weeks, which is the usual timeframe outline for most of the currently approved vaccines.
The researchers used a simulation model based on a "real-world" population of 100,000 US adults, finding that delaying a second dose could prove beneficial if a single dose offers at least 80 per cent protection and if vaccination rates stood at 0.1 per cent to 0.3 per cent of the population per day.
The experts, including from the Harvard School of Public Health in Boston and the Massachusetts Institute of Technology (MIT), calculated the strategy could prevent between 47 and 26 deaths per 100,000 people overall.
The effect was particularly strong for the under-65 age group, where a delayed second dose strategy performed consistently well under all vaccination rates tested.
Watch: Do coronavirus vaccines affect fertility?
The policy of delaying vaccine doses was widely contested at the time that Britain adopted this approach amid a shortage of supplies and surging infections rates.
Many critics argued that the delayed administration of a first and second vaccine dose had not been fully tested during the clinical studies. Advocates insisted the data was there to support the policy, arguing it was the only option available to save as many lives as possible.
“It became clear that, while the bottle-neck was vaccine availability, far more lives could be saved, and hospital and critical care admissions prevented, by providing one dose to as many people as possible, particularly those at highest risk of serious Covid-19 disease outcomes, before providing second doses,” said Dr Peter English, a former chair of the BMA Public Health Medicine Committee.
“This was the basis for the UK decision to delay the second dose until 12 weeks, which has proven highly effective.”
Dr English said that concerns surrounding a supposed lack of evidence on the effectiveness of delaying doses were “misplaced”.
“Everything we already knew about vaccines also tells us that a longer prime-boost interval enhances the breadth and depth of the immune response, giving longer-lasting immunity that is likely to provide greater cross-protection against variant strains.”
Addressing the BMJ research, he said: “This study demonstrates – using modelling – that the same is likely to apply, not just in-country, but globally; that delaying the second dose worldwide will most quickly control the disease.
The authors of the study said: "The results suggest that, under specific conditions, a decrease in cumulative mortality, infections, and hospital admissions can be achieved when the second dose of vaccine is delayed.
"This was most significant when the second dose was delayed in people below 65 years of age, with second doses still prioritised for those over 65.
"The conditions in which these benefits were observed included the first-dose vaccine efficacy being above 70 per cent and vaccination rates remaining below 1 per cent of the population per day."
They added: "Delaying the second dose but prioritising it for people aged under 65 can result in lower mortality rates compared with the standard two-dose strategy, even at vaccination rates up to 1 per cent of the population per day."
Watch: What UK government COVID-19 support is available?
Read More
Political turmoil returns as Nepal suffers worst COVID surge

 Yahoo Finance
Yahoo Finance 