Australian drug shortage sparks calls to loosen prescription rules
The Pharmaceutical Society of Australia has called on the federal government to allow pharmacists to be able to substitute medicines for same drugs of a different brand to address shortages of government-subsidised drugs.
The move comes amid significant shortages of the most widely prescribed antidepressant.
The society also wants pharmacists to provide alternative forms or strengths of a medicine in shortage, when it is appropriate and safe to do so, without the need for approval from the drugs regulator, the Therapeutic Goods Administration (TGA).
Consumers have reported shortages of commonly prescribed drugs such as the contraceptive pill Norimin over the past year. When the brand name or generic is out of stock, patients need to go back to their doctor and get an alternative script, unless the drug is one that the TGA has deemed as being in “serious shortage” in which case pharmacists are allowed to substitute without approval from the prescribing doctor.
Related: Zoloft enters list of 10 most commonly prescribed drugs in Australia
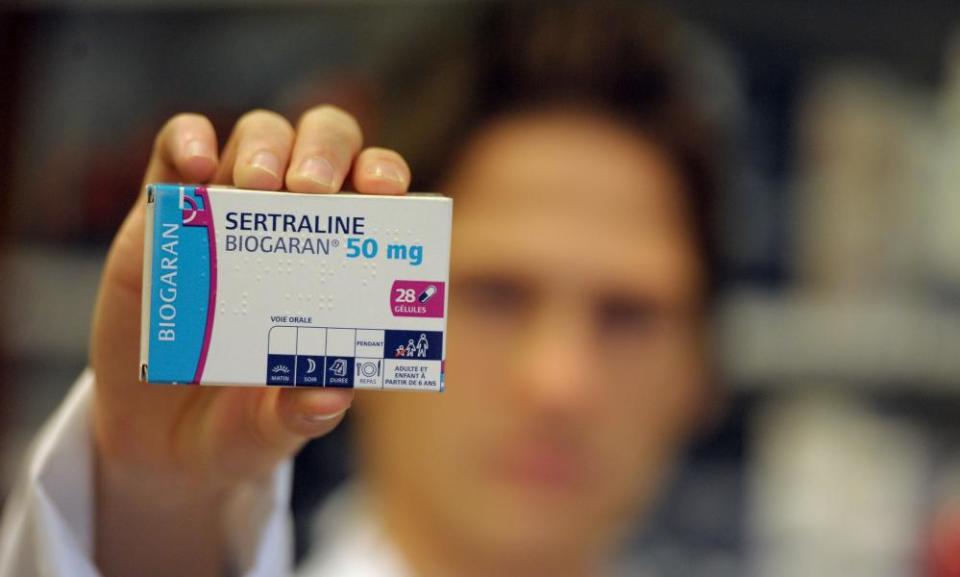
The society says there are significant shortages of one of the most commonly prescribed antidepressants in Australia, sertraline, sold under the brand name Zoloft.
The society’s president, Associate Professor Chris Freeman, told Guardian Australia that a pharmacist may be able to source a non government-subsidised brand from a reputable drug manufacturer.
“However, it may not be covered by the PBS [Pharmaceutical Benefits Scheme], leaving the patient out of pocket, or without the lifesaving medicines at all,” he said.
“Currently, the Pharmaceutical Society of Australia is aware of significant and ongoing shortages of sertraline 50mg and 100mg, which is having considerable impact on patients, particularly from a cost perspective.”
He said the society was working closely with the TGA and Consumers Health Forum on the issue.
Freeman said the society supported comments from Australian Medical Association vice-president, Dr Chris Moy, that more needed to be done by the federal government to address shortages. Moy told ABC Radio Sydney on Wednesday that Australia should boost its ability to manufacture drugs on-shore. The majority of Australia’s most commonly used medicines are produced in India while most ingredients are sourced from China.
“Australia hasn’t proven itself to be very good at making things … we just thought we’d forever be able to just get this whenever we needed, these medications in a continuous supply,” Moy told the ABC. “And that hasn’t proven to be the case.”
Guardian Australia has contacted the federal health minister, Greg Hunt, for comment.
While Moy attributed some of the drug shortages to Covid-19 and lockdowns and border closures, which he said “stress tested” supply chains, a TGA spokeswoman said the number of national medicine shortages experienced in Australia did not increase significantly during the pandemic in 2020.
The average monthly total of new national medicine shortages published on the TGA website was largely consistent with the previous year’s average.
“Most disruptions to medicine supply during the pandemic were confined to local out-of-stocks driven by increased demand at community pharmacies and hospitals,” the spokeswoman said.
Medicine shortages of all prescription medicines and certain over-the-counter medicines are monitored centrally via the TGA’s Medicine Shortages Information Initiative. Pharmaceutical companies must report any impending shortages of these reportable medicines to the TGA.
A Medicines Australia spokeswoman said the medicines supply chain had functioned well with the pandemic and “demonstrated significant resilience”. In response to Moy’s comments, she said the set-up of manufacturing of medicines in Australia is “complex and dependent on many factors many of which are unrelated to cost”.
“Covid-19 has placed a firm spotlight on this issue and all stakeholders are actively considering what a future may look like where local manufacturing can play its role in supporting Australia’s medicine needs,” she said.
“Our industry continues to work around the clock to monitor and assess supplies, locally and globally, and to ensure medicines can get to where they are needed during Covid-19 and beyond.”
In the meantime, Medicines Australia discourages any stockpiling either by patients or by state and territory health authorities.
The chief executive of the Australian Thyroid Foundation, Beverley Garside, said the ATF had reported more issues than usual in the last year regarding supply of their medications to control symptoms and thyroid function in Graves’ disease.
“This year, patients have been told by pharmacists the lack of supply was due to Coronavirus, or the waterfront dispute,” Garside said. “It worries me that pharmacists do not always investigate the reason stock is not available or tell patients versions that may not always be correct.”
Related: Supply delays could threaten start of Australia's Covid vaccine rollout
Garside said when she contacted the drugs sponsor, which is usually a pharmaceutical company, she was told the real reason for supply shortages was border closures, which were causing delays in deliveries.
“It’s not an ideal situation for patients to be placed in, as one of the symptoms of Graves’ disease is anxiety, which of course is always raised when a patient cannot access their medication,” she said.
The CEO of the Consumers Health Forum, Leanne Wells, said universal and timely consumer access to the right medicines for their conditions is a fundamental part of our national medicines policy.
“It’s a right Australians can and should expect,” she said.
“The pandemic has heightened our awareness of medicine supply chains however we have been assured by the TGA that medicine shortages are largely consistent with previous years and that the issue is more of pharmacies being out-of-stock short term than chronic shortage.”
Do you know more? melissa.davey@theguardian.com

 Yahoo Finance
Yahoo Finance 