GPs in England threaten industrial action over in-person appointments
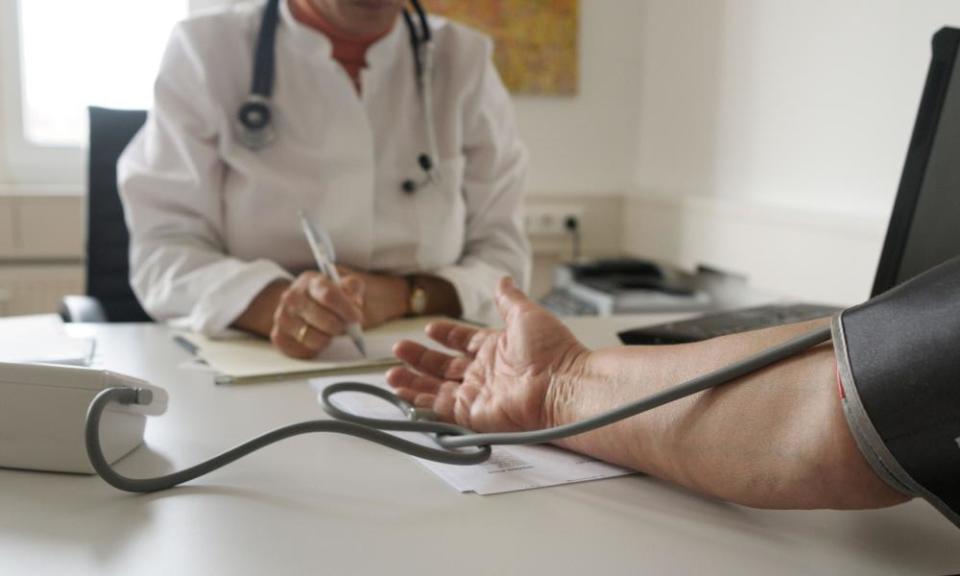
GPs in England are threatening industrial action in protest at the government’s attempt to force them to see any patient who wants a face-to-face appointment.
The British Medical Association’s GPs committee voted unanimously to reject the plan by the health secretary, Sajid Javid, which included “naming and shaming” surgeries that see too few patients in person.
Related: Face off: the government versus GPs
The doctors’ union has decided to hold a ballot on possible industrial action, which could result in family doctors at the 6,600 practices in England reducing the work they undertake.
“GPs have been left with no alternative but to take this action. All efforts to persuade the government to introduce a workable plan that will bring immediate and longer-term improvement for doctors and their patients have so far come to nought,” said Dr Richard Vautrey, the chair of the BMA’s GPs committee.
It is a dramatic escalation of GPs’ increasingly bitter war of words with ministers and comes as soaring Covid cases put increasing strain on the health service.
Watch: GPs condemn ‘abuse’ over in-person care as Javid fails to address conference
It could herald the first major clash between the medical profession and ministers since the year-long junior doctors’ dispute in England in 2015-16, which involved a series of walkouts by trainee medics.
GPs have been angered by Javid’s instruction last week that they should see many more patients in person, and a plan to publish monthly data showing what proportion of each surgery’s appointments occur in person or virtually. They are also frustrated by what they say is a lack of action to reduce their heavy workloads.
Family doctors are also furious at a separate plan to compel those who are paid at least £150,000 a year for NHS work to declare their earnings, announced in 2019 and starting next month. The BMA has said this could imperil family doctors’ safety because “forcing GPs to publish their earnings provides no benefit to patient care, yet will potentially increase acts of aggression towards GPs and will damage morale amongst the profession and only worsen practices’ ability to recruit and retain GPs.”
It is unclear how much of an impact industrial action by GPs would have on the care patients receive. But if family doctors vote to forge ahead, it could lead to GPs:
Declining to comply with Javid’s insistence that they see patients in person who request it.
Visiting care homes less often to check on residents’ health.
Undertaking fewer or less regular medication reviews of the drugs being taken by patients with a long-term health condition.
Refusing to issue Covid medical exemption certificates, which will allow people who remain unvaccinated to continue working in environments such as care homes because they have a medical reason not to have been jabbed against the disease.
The BMA sought to reassure patients by pledging that any changes to usual working patterns would not affect GPs’ involvement in the rollout of either winter flu jabs or Covid booster vaccines. However, the decision has prompted fears that patients could find it harder to see a GP at their surgery.
“This shows the government’s deliberately provocative plans to name and shame GPs has backfired,” said Daisy Cooper, the Liberal Democrats’ health spokesperson. “Sajid Javid must now dial down the rhetoric and get round the table with doctors and patient groups to find a way forward. It would be unforgivable if, as we enter a winter crisis, people are unable to access their local GP.”
Watch: Parents of student claim GP phone consultations cost him his life
The BMA and Royal College of GPs are deeply frustrated that Javid’s plan contained few of their proposed steps to help to reduce GPs’ “unsustainable” workloads.
They had asked him to suspend the Quality Outcomes Framework (QOF) under which surgeries are paid agreed sums for monitoring the health of people with conditions such as asthma and diabetes, saying it takes up too much time and that removing the QOF system in Scotland has not damaged patient care.
It is not certain that GPs will hold a ballot because the BMA’s ruling council has to approve that course of action. But Dr Chaand Nagpaul and Dr David Wrigley, the union’s chair and deputy chair of council, are appalled at Javid’s stance.
Nagpaul has insisted it is the lack of GPs in England – the number of full-time GPs has fallen by 1,800 since 2015 despite a rising population – that has limited rapid patient access, not family doctors’ willingness to see all those seeking a consultation.
Vautry said: “The ultimate outcome should be to end the current crisis in general practice, to properly support practices to manage their workload pressure, including safely getting through the backlog of care caused by the pandemic, and deliver a safe service to patients, allowing time to create an agreed long-term plan to make general practice sustainable for the future.”
A Department of Health and Social Care spokesman said: “We want patients to be able to see their GP promptly and in the way they choose. Our plan will improve access and drive up face to face appointments, it includes providing a further £250m to GPs in order to boost capacity.”

 Yahoo Finance
Yahoo Finance 